Johns Hopkins University has earned a global reputation as a place where lifesaving discoveries take place. But never before has the talent and expertise behind that reputation been as evident—and as urgently needed—as it is during the ongoing coronavirus pandemic.
In mid-March, while the university transitioned to remote learning and telework to encourage social distancing practices and slow the spread of COVID-19, laboratories and research programs across the university were also asked to suspend their operations. But at the same time, Johns Hopkins launched a massive and ambitious initiative to repurpose research facilities and allocate new financial resources to projects that will advance our understanding of COVID-19, prevent its spread, and care for the sick.
"This is a university that lives and breathes research—optimizing and maximizing research is in the very fiber of our being," says Denis Wirtz, vice provost for research at Johns Hopkins. "There are very few universities that can contribute on this scale to addressing the immediate needs of the global community. It's a beautiful thing to be involved in."
To date, $6 million in university funding has been redirected to support roughly 260 scientists and researchers working on 25 projects grouped under five complementary interdisciplinary themes: understanding the virus, understanding and mitigating transmission, understanding the effects of COVID-19 on patients, helping patients recover, and developing new ways to protect health care workers and solve supply chain issues.
The COVID-19 Research Response Program is focused on supporting high impact, foundational projects that provide the framework and resources—including data, assays and samples—necessary to enable further COVID-19 research at JHU. The groups will share initial reports and relevant instructions for accessing shared resources in May.
The projects include a highly publicized—and promising—clinical study that will investigate whether the blood plasma of recovered COVID-19 patients can boost the immunity of frontline health care workers and treat those already infected with the disease. In a related effort, another team is looking at ways of adapting commercial genetic testing kits or glucose monitors to measure COVID-19 antibodies.

Image caption: Helen Xun shows off two forms of ventilator splitters she is helping to design and 3D print
Image credit: Will Kirk / Johns Hopkins University
The initiative also includes projects aimed at understanding the virus on a micro scale, including an effort to sequence its DNA in order to track its spread, as well as programs designed to inform COVID-19 responses at the macro scale, such as the team developing outbreak models to create custom response plans for international government leaders.
Drawing from the institutional expertise of research leadership in several university divisions—a group Wirtz fondly calls his "brain trust"—the newly formed COVID-19 Johns Hopkins Clinical Research Coordinating Committee is reviewing and prioritizing all clinical research relating to the coronavirus, ensuring the teams have access to the laboratories and funding necessary to complete their studies within an ambitious three-month timeframe.
"The focus of these projects is on immediate impact," Wirtz says. "Are we thinking about long-term solutions? Of course. But our main concern is on immediately improving the health of patients, health care workers, and our global community."
The coordinating committee also includes an Emergency Response IRB to streamline the research oversight process and a centralized biospecimen repository that will provide blood, saliva, and other necessary patient samples for research. The biospecimen repository is overseen by Lauren Sauer from the Johns Hopkins Office of Critical Event Preparedness and Response.

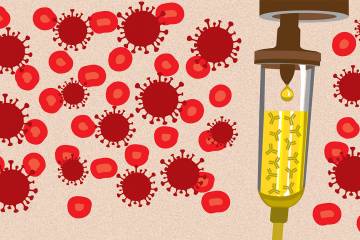
Image caption: Aaron Tobian, a pathologist and director of the Division of Transfusion Medicine at Johns Hopkins Hospital, holds a bag of blood plasma, the focus of a research project that aims to boost the immunity of front line health care workers and treat patients with COVID-19.
Image credit: Will Kirk / Johns Hopkins University
"Johns Hopkins is a leader in research and innovation, so it stands to reason that our faculty and research scientists would not shy away from the urgency of this moment," says Sunil Kumar, Johns Hopkins University provost. "It is thrilling—and a point of pride—to see our community rise to the challenges presented by the coronavirus and work together and across disciplines to develop solutions that will keep the world safer and healthier."
Understanding the virus
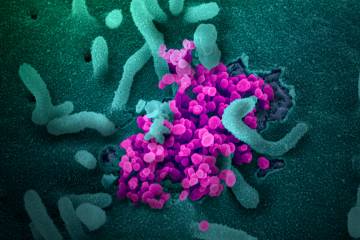
Johns Hopkins research teams are undertaking several efforts to study SARS-CoV-2, the virus that causes the illness COVID-19. A collaborative team of geneticists, engineers, and epidemiologists is working to create genetic sequences of hundreds of virus samples collected in the Baltimore region. Under the direction of team leaders Stuart Ray and Winston Timp, the team is tracking how the virus mutates person-to-person and case-to-case in an effort to understand community transmission of the disease. Based on current data, the team has observed that parts of the virus targeted by vaccine developers are genetically stable. This is strong evidence that a successful vaccine will provide protection against COVID-19 without needing to be updated over time.
Understanding and mitigating transmission
Several interdisciplinary teams are working to understand how the virus moves from person to person and to help curtail that transmission.
One program, led by Garry Cutting and Sharon Gerecht, aims to develop and deploy population-level testing through two potential routes: creating a diagnostic test that involves minimally-invasive oral fluid collection (similar to the sample collecting methods of genetic test kits such as 23andMe), and adapting commercial glucose sensors to measure COVID-19 antibodies.
Shruti Mehta, Jason Farley, and Jacky Jennings are leading another team in an effort to deploy nationwide telephone and online surveys and tap into existing study cohorts in Baltimore to carry out a population-based investigation that seeks to understand and measure the social, economic, and health impacts of COVID-19, as well as the effectiveness and consequences of the strategies used to prevent its spread.
Others are working to develop modeling systems that can better inform policymakers as they weigh social, economic, and public health decisions on the local, state, and national level. This project, led by Kate Grabowski, David Peters, Daniel Polsky, and Tom Burke seeks to support critical services such as time-sensitive advice and custom-made reports that will help governments and other entities understand their epidemic data and assess their policy options. This project includes support for the popular Johns Hopkins COVID-19 tracker map and other data visualization efforts.
Finally, a fourth team is investigating how the virus spreads through communities of health care workers while they provide medical services and when they put on and remove personal protective equipment such as face masks. This program, led by Allen Kachalia, Kathy McDonald, Richard Rothman, and Tener Veenema, aims to develop risk-mitigation strategies to protect the health and safety of these frontline medical providers. They are also creating mental health and social support resources for health care workers operating under trying circumstances.
Understanding the effect on the patient
Priya Duggal, David Kass, and Chirag Parikh are leading an effort to study the mechanisms that underlie the high mortality of COVID-19 infection in certain subgroups, with the goal of rapidly developing an intervention to change this outcome. The team will identify biomarkers and risk factors among these subgroups to inform clinical decision-making and evaluate different therapeutic options. They will assess the cellular, tissue, and host responses from a signaling and immunological context.
Another team, led by Justin Bailey, Andrea Cox, Diane Griffin, Ben Larman, and Andy Pekosz, is working to define the immune responses and antibodies associated with COVID-19 recovery and severe illness resulting from the disease. This line of research has critical implications for understanding what factors help patients recover from infection and how they might be protected from re-infection, as well as understanding how to prevent future outbreaks.
Helping patients recover
The therapeutics program, led by Mark Sulkowski and Paul Auwaerter, is creating the critical infrastructure necessary to implement human vaccine trials in ambulatory and hospital settings through a new COVID-19 Clinical Research Core, and will support promising new therapies through a COVID-19 Preclinical Novel Therapeutic Drug Working Group. One of the project teams is working to develop and deploy a treatment that uses the blood serum containing the antibodies of recovered COVID-19 patients to boost the immunity of at-risk health care workers and to treat sick patients. Led by Arturo Casadevall, the team of physicians and scientists have established a network of hospitals and blood banks that can collect, isolate, and process blood plasma from COVID-19 survivors. Under the FDA's emergency compassionate use authorization, the first patients were treated in Houston and New York City in early April, and several clinical trials are in preparation.
Innovating to protect health care workers and solve supply chain issues
A team of engineers are hosting a series of "sprint cycles" and hackathons with health care subject matter experts to address high priority challenges such as critical supply chain shortages, equipment repurposing, and novel device design and fabrication. The group has already held a five-day, student-run online design challenge to develop innovative solutions to a range of problems posed by the COVID-19 pandemic. Led by Nicholas Durr, Alan Ravitz, and Youseph Yazdi, the team is also supporting an effort to develop and prototype a 3D-printed splitter that will allow a single ventilator to treat multiple patients safely and effectively, and a pumpless ventilator that can run on pressurized air and a 12-volt battery.
Anyone who would like to loan their skills, equipment, supplies, or space to these projects is asked to fill out the associated interest intake form on the Johns Hopkins COVID-19 Research Response Program website. These entries are shared with the team leads regularly.
Researchers interested in understanding the landscape of COVID-19 research at JHU, who need assistance locating resources, or who would like to subscribe to the weekly funding opportunities listserv should send inquiries to resapp@jhu.edu.
Correction: An earlier version of this article overstated the implications of the findings from the genomic testing group regarding the potential effectiveness of a one-time vaccine. The Hub regrets the error.
Posted in Health, Science+Technology, University News
Tagged interdisciplinary research, denis wirtz, biomedical research, sunil kumar, coronavirus, covid-19