- Name
- Jill Rosen
- jrosen@jhu.edu
- Office phone
- 443-997-9906
- Cell phone
- 443-547-8805
The Johns Hopkins University's Coronavirus Resource Center is launching the Pandemic Data Initiative as a new resource to spotlight systemic deficiencies in the collecting and reporting of pandemic data, to examine how those challenges hinder COVID-19 responses, and to explore possible solutions to improve public data.
Since the pandemic's start, Johns Hopkins University experts at the Coronavirus Resource Center had a behind-the-scenes view on how state, federal, and global agencies collected and reported COVID-19 data. Their analyses revealed a troubling truth: In the absence of standards and uniform methods, the states used an uneven patchwork of policies and disjointed reporting that hampered efforts to slow COVID-19's spread, sowed confusion for policymakers and the public, hindered the ability to target resources to the most vulnerable, and complicated the process of measuring the effectiveness of public health interventions and vaccinations.
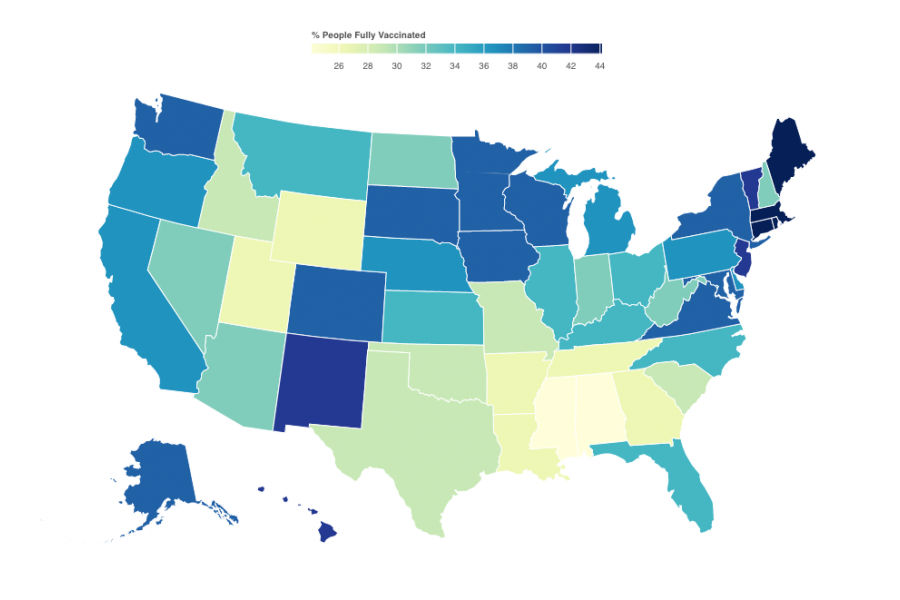
Variations have emerged in all aspects of coronavirus data, including how to report testing results, track vaccination distribution, determine confirmed case, and classify confirmed deaths. Among the most troubling aspects has been a lack of demographic data to fully illustrate the disproportionate impact of COVID-19 on minority communities and how resources for medical care and vaccinations were not equitably distributed.
Also see
Inconsistent data practices continue to stymie efforts to bring the pandemic to an end. For example, as states begin to relax policy decisions such as mitigation measures and masking requirements based on increasing vaccination rates, the Pandemic Data Initiative has identified concerns about how those rates are calculated—especially since states began counting the Johnson & Johnson single-dose vaccine along with the two-dose regimens of Pfizer and Moderna. Ohio and Mississippi, for example, have been counting the J&J shots under two different categories, making it nearly impossible to precisely calculate the total number of people partially and fully vaccinated.
"There is a lot of complexity in the way COVID-19 data has been collected and reported that we haven't been able to fully contextualize because of a lack of uniformity in how state and federal agencies manage it," says Beth Blauer, associate vice provost for public sector innovation and the CRC data lead. "The PDI aims to explain how the data got to where it is and explore the opportunities for creating more high value public data sets."
This new initiative will continue to harness the public health expertise of the Johns Hopkins Bloomberg School of Public Health, along with the many months of deep research and hands-on data science that have become the hallmark of the CRC's work. The CRC experts who have been at the forefront of calls for improved public data will contribute to the PDI, including:
- Beth Blauer, CRC data lead, associate vice provost for public sector innovation;
- Jennifer Nuzzo, CRC epidemiology lead, associate professor in the Johns Hopkins Bloomberg School of Public Health's Department of Epidemiology, and senior scholar at the Johns Hopkins Center for Health Security;
- William Moss, CRC vaccinology lead, executive director of the International Vaccine Access Center, and professor in the Johns Hopkins Bloomberg School of Public Health's departments of Epidemiology, International Health, and Molecular Microbiology and Immunology;
- Brian Garibaldi, CRC clinical lead, medical director of the Johns Hopkins Biocontainment Unit, and associate professor of medicine;
- Lauren Gardner, chief architect of the CRC's global dashboard, director of the Center for Systems Science and Engineering in the Johns Hopkins Whiting School of Engineering.
The Pandemic Data Initiative will feature a new blog and regularly updated analysis spotlighting data challenges and irregularities, as well as expert discussions that will contemplate possible solutions for ongoing COVID-19 pandemic management and future public health crises.
Posted in Health, Science+Technology, University News, Politics+Society
Tagged data, coronavirus, covid-19, coronavirus resource center