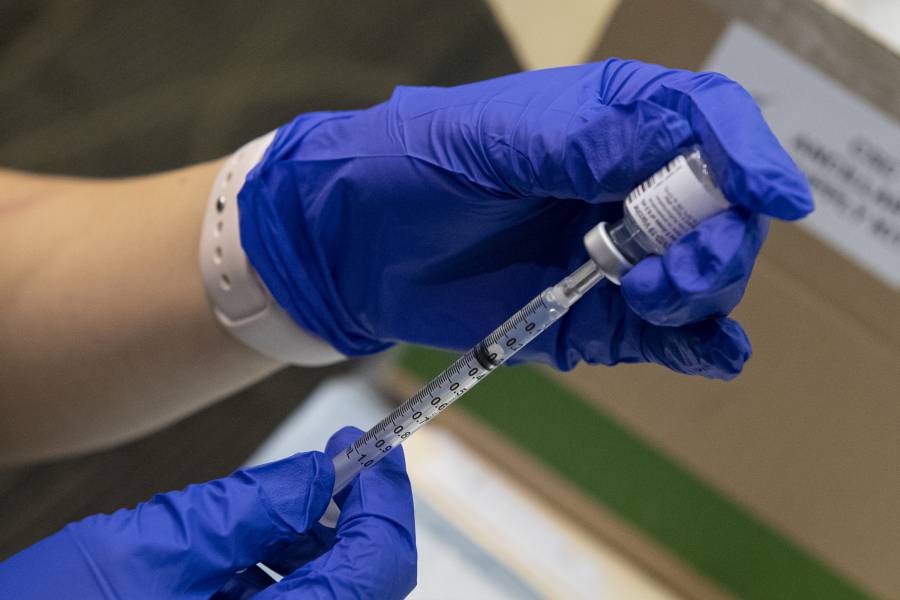
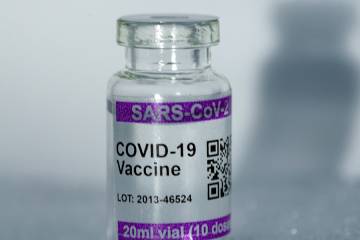
It's been three weeks since the COVID-19 vaccines began arriving at hospitals, clinics, and pharmacies. Operation Warp Speed—the U.S. vaccination development, testing, and distribution effort—had made 20 million vaccine doses available by the end of 2020. Yet the U.S. is only approaching 5.5 million vaccines administered so far.
Public health experts, policymakers, and the leaders of Operation Warp Speed agree: The U.S. must pick up the pace of vaccination.
For a closer look at the state of COVID-19 vaccination in the U.S., the Hub turned to Tinglong Dai, an associate professor at the Johns Hopkins Carey Business School. An expert in operations management and health care analytics, Dai has closely followed the rollout of vaccines in the U.S. and shares insights on what's working, what needs to be improved, and how the fractured and decentralized U.S. health care system might be able to prepare for future national health care crises.
What is the current state of the vaccination effort in the U.S.? Are we where we wanted to be or expected to be when vaccine distribution began last month?
We are experiencing the initial hiccups of vaccine distribution. Everyone is learning to appreciate the difficulty of getting the vaccines administered into people's arms. We will almost certainly do better in a month or two, except that we don't have the luxury of taking the time to perfect things. After all, we have hundreds of thousands of infections and thousands of deaths every day.

Image caption: Tinglong Dai
Expectations also matter. This time last year, this novel virus was on almost nobody's radar. The fact that we're now talking about vaccination—not just that vaccines are available—is incredible. The Pfizer vaccine has only been approved weeks ago, and the Moderna vaccine was approved just before Christmas. We know things are slow during holidays, so expectations were low.
But whatever those expectations were, what we have achieved is far lower when it comes to administering vaccines. Operation Warp Speed has only shipped about half of its doses. Of those shipped doses, only 30% have been administered. In other words, we are utilizing only 15% of what we as a nation have. We have to do better than this for the U.S. to move on from being the epicenter of the COVID-19 pandemic.
What have been the greatest hurdles to distribution that you've seen?
A supply chain is basically a flow of things. How fast things flow in the supply chain depends on its bottleneck, which can shift from time to time. Right now, the bottleneck of the vaccine supply chain appears to be resources needed for administering the doses. Giving COVID-19 shots is different from giving flu shots—you have to ensure social distancing, have enough personal protective equipment, and people need to be observed for 15 minutes after getting a shot. Not to mention the Pfizer vaccine has a very specific storage requirement and has to be thawed and diluted before being administered. The Moderna vaccine is easier to store, but still requires cold storage. At this time, we simply don't have enough staffing, space, and time to give shots quickly.
Of course, there are other hurdles. One is that both the federal government and hospitals are holding back doses. The federal government does this to ensure enough second doses. Likewise, some hospitals are also holding back doses because they worry second doses may not arrive on time. When doses get stuck in warehouses and freezers, we have a slow-moving supply chain.
Another factor is related to nursing homes. We have about 2 million nursing home residents and staffers in the United States, and we have more doses than needed—we could, if we wanted to, vaccinate all nursing homes in a matter of days. But some states now say they need additional weeks or months to get this done. What has happened is that most of them participate in the Federal Pharmacy Partnership, which relies on CVS and Walgreens networks to vaccinate nursing homes. Unfortunately, the CVS/Walgreens program has turned out to be much slower than expected, owing to limited staffing and paperwork issues that were not addressed in advance. In Maryland, by Jan. 5, CVS and Walgreens had only administered 14% of doses for nursing homes.
What else accounts for that disparity between doses received and doses administered, and how can it be corrected?
States that are doing well tend to have strong statewide coordination and broad participation of various stakeholders. For example, West Virginia leads the nation for vaccinating nursing home residents and staffers. What they have done differently is that they chose not to participate in the Federal Pharmacy Partnership. Rather, West Virginia leaders used their organizational skills and connections to mobilize all the chain and independent pharmacies, not just CVS and Walgreens, to partner with nursing homes. And they used the two-week waiting period after the FDA authorization of the Pfizer vaccine to do what it takes to match supply and demand. Unfortunately, most other states chose a passive approach and allowed small problems to turn into bigger ones.
Also see
To correct the situation, states and local authorities need to take proactive actions and set up the widest possible network of distribution sites as more doses are available. As in the case of West Virginia, we need to engage all chain and independent pharmacies and standalone clinics who are capable of administering vaccines.
Our vaccine supply chain is as inequitable as it is slow-moving. To address that, we should establish Amazon-style fulfillment centers at the state and county levels that receive shipments from the feds and deliver vaccines to various distribution sites on an on-demand basis or following a given schedule. Think about it—Amazon can deliver to 70% of the U.S. population on the same or next day. That's efficiency and equity achieved at the same time. Amazon's success relies on a network of fulfillment centers, which pool supply of and demand for millions of items. We need to create Amazon-style fulfillment centers that can deliver vaccines to sites where they are needed. This would help ensure that distribution sites holding back doses will not receive more doses. As we speed up our vaccine supply chain, we must also help distribute vaccines in a truly equitable sense.
We have to rethink how we connect vaccines and people. When we hear the story of a 71-year-old woman who made 184 calls to get a vaccine appointment and failed, we know there's something fundamentally wrong with our vaccine supply chain. Finding when and where to get vaccines isn't supposed to be as hard as it is now. Large providers like Johns Hopkins use secure patient portals like MyChart to schedule vaccine appointments, but many local health departments are using sites like Eventbrite and SignUpGenius. We have such a patched system that I fear many people, especially the vulnerable groups, will be missing out. The systems connecting vaccines and people are so poorly designed—if designed at all—that people have to work super hard to find vaccines. That's not how you speed up the flow of things in a supply chain.
We are a nation with some of the most efficient supply chains on the earth, and we can do better. At a minimum, each state or local authority should offer a cross-provider portal that helps people verify their eligibility and schedule appointments with all the options at hand.
The U.K. has decided to administer single doses of vaccine to more people and to delay the four-week booster shot that is recommended. This strategy has been likened to a wartime decision—one that reflects necessity rather than best practices. U.S. officials, including those who spearheaded Operation Warp Speed, have come out against this strategy. Do you think the strategy has merits, and should it be adopted here in the U.S.?
The U.K.'s strategy has its merits as it will allow more people to get their first doses. In the case of the U.S., our bottleneck at this moment is not really the supply, but the resources needed for administering what we have. I think we should stop holding back the second doses to an unnecessary extent. Vaccine manufacturers are ramping up their production capacity, and we will almost certainly see an upward supply curve. Also, we can always prioritize those who have received the first doses over those who haven't when it comes time to administer booster shots. For these reasons, I think we should stick to the standard two-dose schedule, especially because we can actually do it well by better utilizing our existing resources. We may need to hold back second doses when the general public has access to vaccines—when the supply curve flattens because demands increases, but not now. Let's focus on fixing our vaccine supply chain and moving things faster.
Posted in Health, Voices+Opinion, Politics+Society
Tagged business, coronavirus, covid-19 vaccine