"Using a glue gun wasn't in the curriculum, but I figured it out," says Lukas Mees, squirting a squiggle of glue across an 8-by-11 inch rectangle of clear plastic. A third-year Johns Hopkins medical student, Mees was slated to start his surgical rotation in a few days, but then the coronavirus outbreak hit, and the Association of American Medical Colleges recommended that medical students suspend all patient contact for at least two weeks. Now, the doctor-in-training is among 50 volunteers from across Hopkins gathered at a warehouse in Southeast Baltimore to use scissors, glue guns, and staplers to manufacture plastic face shields for clinicians.
"It's really important for doctors to have the right protective equipment, especially with a virus like this, and there are shortages everywhere," Mees says, between glue squirts. "They don't want us taking direct care of patients who have the virus, so I was just looking for another way to help."

Image credit: WILL KIRK / JOHNS HOPKINS UNIVERSITY
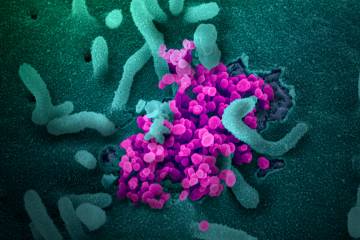
Among the many health challenges presented by the global COVID-19 pandemic is a critical shortage of personal protective equipment—or PPE—such as masks, gloves, and isolation gowns for medical personnel. Most PPE is sourced from China, where the virus has both dramatically reduced production and diverted output for domestic use. Burton Fuller, vice president and chief supply chain officer of the Johns Hopkins Health System, knows this scarcity all too well, through his own experiences and through conversations he's had with medical supply colleagues in virus-ravaged Seattle, where a crush of contagious patients taxed the city's supply of single-use PPE. "They told us that they went through a month's worth of PPE in under a week," he says. "They were talking about 600% increases in usage. This is going to be a dramatic problem for our infection control, and it means we need to get creative."
The face shield project grew out of Fuller's discussions with staff from the Hospital's Department of Hospital Epidemiology and Infection Control who, during an overseas humanitarian intervention, had seen health workers cobble together protective face shields using exposed X-ray film instead of plastic. Fuller began to wonder: Could his department do something similar? The question fell to Michelle Azotea, Johns Hopkins Medicine's director of project management and implementation, whose first phone call was to a local plastic supplier. (No need for the X-ray film route.) "I built a prototype face shield at home on my coffee table," she says. Hopkins infection control clinicians reviewed it and gave it their approval. Then came the following query: "Okay, can you make 50,000 more?"
Each shield is composed of a rectangle of flexible clear plastic, a strip of foam that presses against the wearer's forehead, and an elastic band going around the head to hold it in place. Azotea was able to source the raw materials either locally or through Amazon. A sign-up website was created, and Burton put out a request for volunteers via numerous Hopkins-affiliated email listservs. "We have asked for 50 volunteers, twice a day, to come in and help us assemble these," Azotea says. The response was so great they added two additional 4-hour shifts and are now producing about 5,000 shields a day. Right now, all shields are destined for usage at Johns Hopkins, but Azotea has shared shield-making instructions with other health care facilities.
The need to follow social distancing guidance has complicated the mass production effort. Fortunately, the Consolidated Service Center, where the production line was set up, moved into expansive new facilities two years ago and has 48,000 square feet of space available—room enough for 70 folding tables set 6 feet apart. During each four-hour shift, volunteers remove a protective film from the clear plastic, cut strips of foam out of large rolls, glue the foam to the plastic, and staple an elastic band to complete a shield. The shields are added to a Personal Protection Pack: fanny packs (many donated by Baltimore sports apparel maker Under Armour) that also hold a fabric face mask, hand sanitizer, and a paper bag and marker clinicians can use to label and store their equipment.
Among the volunteers assembling the packs is Beth Stierman, who, when interviewed, had worked every shift since the call for volunteers began March 18. "We're in a pretty trying time, and this seems like something that we can do to help out our frontline health workers," says Stierman, a PhD student in JHU's Bloomberg School of Public Health. "I am actually in international health, so most of my work involves health system issues in sub-Saharan Africa. I don't think anyone expected that we would run out of equipment in the United States. But anywhere you are in the world, people will find ways to help out and end up doing things they never would have expected to be doing.
"It sort of reminds me of World War II, when you heard about Rosie the Riveter," Stierman adds. "People went into the factories who wouldn't have usually been doing that kind of thing."
Rosie the Glue Gunner, perhaps?
Volunteers are being sought daily through April 10. Sign up online.
Tagged pandemic, coronavirus, volunteers, ppe, covid-19, medical supplies