- Name
- Robin Scullin
- rsculli@jhu.edu
- Name
- Barbara Benham
- bbenham1@jhu.edu
Childhood deaths from two leading bacterial causes of pneumonia, meningitis, and sepsis declined sharply during the period 2000 to 2015, especially as vaccines against these pathogens were introduced in high-burden countries, according to new estimates from a team led by scientists at the Johns Hopkins Bloomberg School of Public Health.
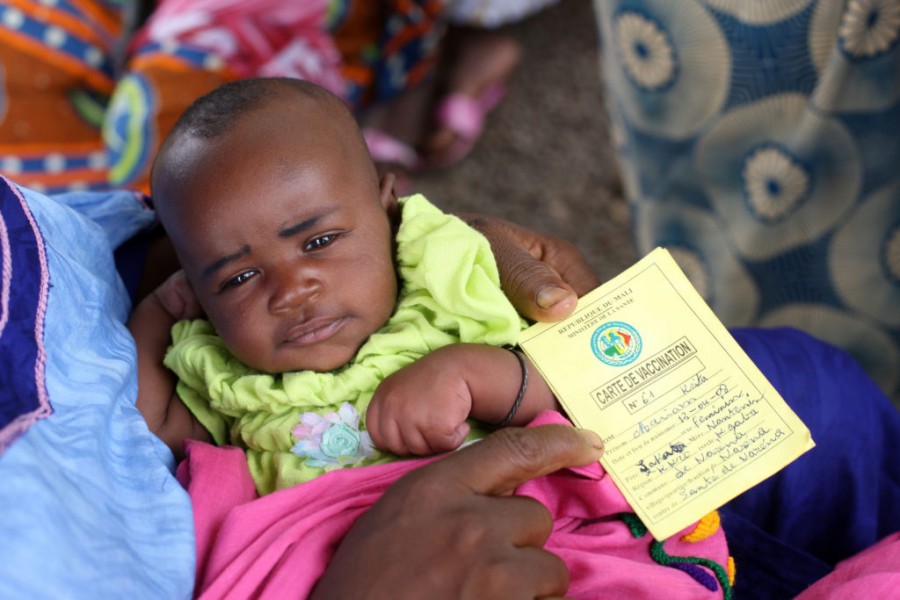
Haemophilus influenzae type b, commonly called Hib, and Streptococcus pneumoniae (called pneumococcus) are bacteria that can cause meningitis, pneumonia, sepsis and other serious complications, especially in children. Conjugate vaccines against Hib have been used in the United States, Europe and some other countries for almost three decades, but children in several developing countries with high disease burdens have only started to receive the Hib vaccine in the past decade and the pneumococcal conjugate vaccine (called PCV) in 2009.
Researchers estimate that between 2000 and 2015, Hib vaccines prevented the deaths of 1.2 million children and PCV prevented about 250,000 deaths.
The findings, published online in The Lancet Global Health, highlight the success of the global fight against these illnesses, and also provide a clear picture of the remaining disease burden, now largely concentrated in South Asia and Africa.
"Further progress against these diseases will depend on efforts in a few large countries," says study lead author Brian Wahl, an assistant scientist at the International Vaccine Access Center in the Bloomberg School's Department of International Health. "These bacteria still cause far too many child deaths."
Wahl and colleagues developed updated estimates of the numbers of Hib and pneumococcal disease cases and deaths in children on a country-by-country basis for each year from 2000 to 2015. They used country-specific data and field-based evidence on the number of child deaths caused by pneumococcus and Hib and compared that data to World Health Organization and UNICEF estimates of vaccine coverage.
Estimates for the year 2000 showed that Hib contributed to about 299,000 child deaths and 2.1 million severe infections, and that pneumococcus contributed to about 600,000 child deaths and 6.6 million severe infections. In 2015, there were approximately 29,500 child deaths linked to Hib and an estimated 294,000 child deaths linked to pneumococcus. These figures suggest declines of 90 percent and 51 percent, respectively, from the estimated deaths in the year 2000. The researchers also estimated that Hib and pneumococcal deaths among children with HIV/AIDS also declined sharply—75 percent—from about 95,000 in 2000 to about 23,000 in 2015.
The sharp declines in child mortality from Hib and pneumococcus were due not just to the introduction of vaccines but also to general factors that have reduced pneumonia and meningitis deaths from all causes, such as better hygiene and access to health care. "In 2015 compared to 2000, fewer children died from all causes, not just Hib and pneumococcus," Wahl notes.
However, there was evidence that vaccines were specifically responsible for a considerable reduction in mortality. "The estimated average annual decline in child deaths from pneumococcus jumped from 3 percent during 2000-2010 to 8 percent after 2010 when many high-burden countries began widespread immunizations with PCV," Wahl says.
The new estimates will guide ongoing efforts to reduce the burdens of Hib and pneumococcal diseases, which together still kill approximately 900 children per day around the world. The estimates suggest, for example, that about half of the pneumococcal child deaths in 2015 occurred in just four countries: India, Nigeria, Democratic Republic of the Congo, and Pakistan.
"The pneumoccocal disease burden is now limited to a small number of countries that have not introduced the vaccine or have not yet fully scaled the vaccines," Wahl says.
Posted in Health
Tagged global health, vaccines, international health