Debates over the efficacy of convalescent plasma as a treatment for COVID-19 are normal and productive parts of scientific discussions, Johns Hopkins immunologist Arturo Casadevall suggests in a new Wall Street Journal op-ed.
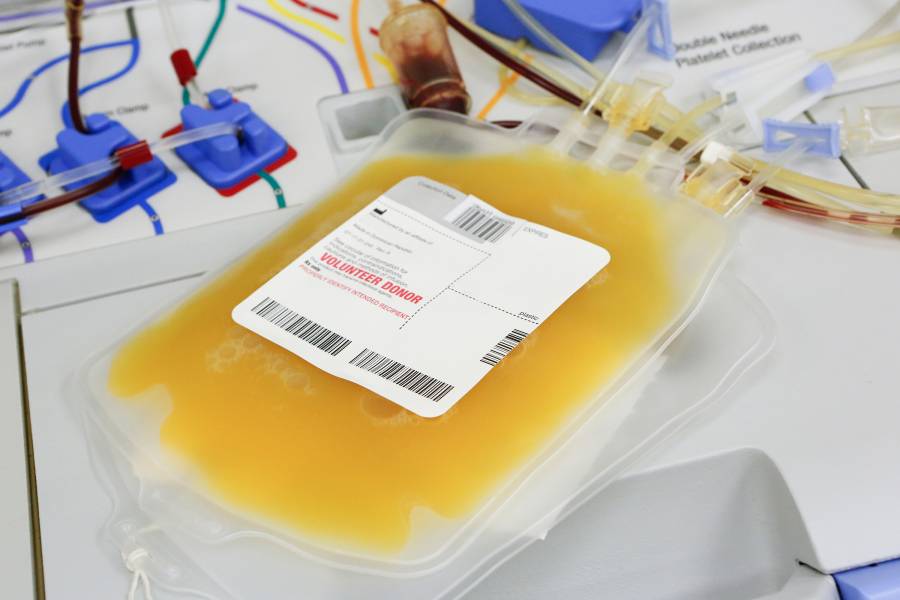
Casadevall co-authored a study on convalescent plasma that helped the U.S. Food & Drug Administration reach its Aug. 23 decision to authorize emergency in-patient use of the treatment, which extracts antibodies from the blood of recovered COVID-19 patients to boost the immunity of those at risk. The authorization ignited something of a media firestorm, with some claiming that President Donald Trump's administration—using disputed statistics—was politicizing science in pushing for convalescent plasma.
Then earlier this month, a National Institutes of Health panel appeared to contradict the FDA decision, stating that data were insufficient "to recommend either for or against" use of plasma.
In The Wall Street Journal, Casadevall—along with co-author Nigel Paneth, an epidemiologist from Michigan State University—break down the contradictory responses. "Both agencies were doing their job," they conclude, characterizing this as "a dispute over scientific certainty, which for scientists is normal fare."
Casadevall—a Bloomberg Distinguished Professor of molecular microbiology and immunology and infectious diseases at the Johns Hopkins Bloomberg School of Public Health and School of Medicine—has been a leading proponent of convalescent plasma during COVID-19, pointing to the treatment's past successes countering epidemics like measles and the mumps. Both Casadevall and Paneth are part of national effort, sponsored by the Mayo Clinic working to expand and investigate the therapy's use in the pandemic. The FDA granted initial approval in March for limited uses of convalescent plasma, and in April helped support the launch of the Mayo Clinic program.
Hundreds of hospitals and more than 1,000 physicians have since administered convalescent plasma on hundreds of thousands of patients, Casadevall and Paneth write, with scientists mining this data to study the treatment's efficacy. In the op-ed, they summarize what they've learned:
First, consistent with everything known about plasma, treatment early in the course of disease was critical. Second, in patients treated early, mortality rates were lowest when plasma contained high levels of antibodies, highest in patients who received low antibody plasma, and intermediate when levels of antibody were in the middle.
This "dose response" effect is powerful evidence of efficacy that is difficult to dismiss. These findings, together with animal data, evidence of efficacy from several small studies and good safety data based on 20,000 treated patients in the Mayo Clinic study, led the FDA to issue its Emergency Use Authorization. The NIH, aware of many times when efficacy data from small trials were later disproved by randomized trials, urged caution.
Under normal circumstances, a new medical treatment is approved only after at least one large-scale, randomized controlled trial proves its efficacy without harmful effects. For those who believe in the absolute necessity of such trials before any treatment can begin, the evidence may not yet support the FDA's recent action, Casadevall and Paneth acknowledge. The authors describe themselves as "ardent proponents of randomized controlled trials" and their continuance during COVID-19, but say they're also willing to trust "observational studies" to inform medical knowledge and practice.
"Where scientists stand in this controversy may reflect their individual approaches to the certainty of knowledge," they write. "This is a healthy debate."
Read more from The Wall Street JournalPosted in Health, Science+Technology, Voices+Opinion
Tagged arturo casadevall, coronavirus, covid-19, convalescent plasma