In her earliest days in Baltimore, Mónica Guerrero Vázquez traveled on city buses without a specific destination, loosely in search of connections. Born in Ecuador, Guerrero Vázquez had recently moved from Madrid, leaving behind the country's economic crisis in hopes of a job to pair with her computer science degree. And to find stability.
The obstacles were great, however. Guerrero Vázquez wasn't an American citizen, her English skills were choppy, and she had no access to health care.
Through her wanderings, she met strangers who became allies. Eventually, she stitched together a support network of nonprofits, charities, and churches that served Baltimore's ever-growing community of Spanish-speaking people. "I connected with a lot of immigrants, and I don't know how to describe it—it was beautiful," she says. "It was like finding my identity, finding people who looked like me and spoke Spanish like me."
The Esperanza Center, run by Catholic Charities, helped Guerrero Vázquez access health care via a program at Johns Hopkins, and she ended up volunteering in legal services there. Through those introductions, she also volunteered for a health literacy program run by a Johns Hopkins Bayview Medical Center resident, giving presentations in Spanish on nutrition and health at local churches.
Turned out that Guerrero Vázquez circled the orbit of Hopkins at an opportune moment. Around that time, a group of Spanish-speaking clinicians and medical faculty realized they needed a more coordinated response to Baltimore's Latino immigrant community, which had a disproportionate rate of conditions like diabetes, obesity-related diseases, high blood pressure, and depression but faced difficulty navigating the health system. In many cases, they avoided medical attention entirely until their needs became dire.
Guerrero Vázquez met two women at Hopkins she later learned "were a big deal," as she puts it: Kathleen Page, an associate professor of medicine with a specialty in HIV/AIDS and infectious diseases, and Sarah Polk, an associate professor of pediatrics and director of the Children's Medical Practice clinic. The pair were launching an effort dubbed Centro SOL and in the summer of 2013 hired Guerrero Vázquez to be its program coordinator. Over the next few years, the three women and their colleagues built Centro SOL into a centerpiece of Baltimore's Latino community, extending services that today include mental health groups and mentoring, teen enrichment, maternal health support, research on Latino health needs, and outreach and advocacy.

Image caption: From left: Sarah Polk, Mónica Guerrero Vázquez, and Kathleen Page
Image credit: Courtesy of Mónica Guerrero Vázquez
More concept than meeting place, Centro SOL—short for the Center for Salud (Health) and Opportunity for Latinos—has never actually had a physical home, apart from a small corner office at Johns Hopkins Bayview, and its only paid staffer is Guerrero Vázquez. The center is instead a loosely coordinated group of people—a bilingual team including physicians, nurses, scientists, social workers, and a growing cadre of community health workers—who, as Polk says, "are committed to a deeply held vision of advocating for more responsive health care for Latinos."
It took Guerrero Vázquez a while to recognize the direction her career was taking. Thinking of herself as a computer engineer who had landed in program management, "I didn't even really realize I was working in public health," she says. She was genuinely surprised when colleagues encouraged her to apply for the Bloomberg American Health Initiative Fellowship and to pursue her master's in public health at Hopkins—both of which she ultimately did, along with becoming Centro SOL's executive director in 2019.
When Centro SOL launched, some were skeptical that such a resource was even warranted. In many people's minds, the racial identity of Baltimore is literally black and white, Polk says. "There was at first plausible deniability about the prevalence of the Latino community," she says.
Census numbers show otherwise. Between 2010 and 2020, Baltimore's Latino population exploded by 134%. Since then, it has risen by another 77%. The trends in Baltimore mirror national patterns, with Latinos now making up nearly one in five people in the U.S.—the country's largest racial and ethnic minority group, expected to constitute more than 26% of the population by 2050. In 2020, that growth helped overturn Maryland's majority-white demographics for the first time.
What's unusual about Baltimore's dynamic is that the rise of Latinos runs counter to the trends of the city's overall population, which has declined steadily for decades. As many major U.S. cities boomed with a so-called urban renaissance in the decade starting in 2010, Baltimore lost 35,000 residents, reaching its lowest population levels of a century in 2020. "Other groups are leaving, and this group is staying, and that in itself is worth considering," Polk says.
The factors behind Baltimore's Latino surge are complex and many, but political environment is surely one. Maryland is known as an immigrant-friendly state, and for Baltimore, welcoming immigrants has been an explicit policy goal. In the early 2010s, then Mayor Stephanie Rawlings-Blake pointedly encouraged immigrants to move to Baltimore in an effort to stem population bleed and boost the city's coffers.
Many immigrants have arrived from Mexico or Central America, fleeing violence or seeking economic opportunities. The East Coast corridor promises such options, and Baltimore sits centrally between D.C. and Philadelphia but with markedly lower housing costs than those two cities. Much of the Latino population is clustered in and around Southeast Baltimore, including the historically diverse Highlandtown, a neighborhood of rowhouses, corner stores, and bars, with the Sacred Heart of Jesus Church serving as a community anchor. Surrounding neighborhoods including Fell's Point, Greektown, and Patterson Park have also seen growth in their Latino populations, as have areas around Johns Hopkins Bayview.
For medical professionals at Hopkins, these population trends became obvious in clinical practice in the aughts. Latino patients were showing up more frequently, Polk says, most commonly in obstetrics, pediatrics, and HIV treatment, owing to programs or federal laws that allowed them direct access to those platforms of care regardless of citizenship status.
But doctors from different specialties were "really struggling to provide the same level of care" to this population as to their nonimmigrant patients, Polk says. With many Latino patients lacking English fluency, health insurance, and reliable transportation, logistical hassles could easily become boulders. Referrals would often die in process, and prescriptions would go unfilled.
Polk remembers one patient, a child born in Mexico who came to Baltimore with her large family, including a "very resourceful, determined mother with essentially no formal English." Polk needed to refer the child to a neurologist, a fairly straightforward process for any English-speaking patient with insurance, but one riddled with complications for this family. "There was no Spanish available to them on the phones or with the staff, no way for them to make an appointment or set up their prescriptions," she says. "The infrastructure just wasn't there."
According to Page, physicians were also noticing a pattern of physical ailments without clear cause. "Latino patients were presenting with a lot of different complaints—headaches, abdominal pain, pelvic pain—but we were often coming up short with diagnoses," she says. But when she pressed patients on mental health issues like trauma or stress, "that would open a whole can of worms."
Eventually, enough doctors, faculty, and staff—across Bayview and in East Baltimore—were talking about these problems that they recognized the need to unite. In 2008, a group of them formed HOLA, which Polk describes as a "kind of faculty affinity group, sharing best practices and commiserating."
Centro SOL ultimately developed as an outgrowth of that movement, as a formal entity with funding from the Levi Strauss Foundation matched by Johns Hopkins. Along with Page, Polk, and Guerrero Vázquez, the center's leaders were Barbara Cook, then medical director of TAP (The Access Partnership), a program providing uninsured residents with low-cost care at Johns Hopkins hospitals, and School of Medicine faculty members Tina Cheng and Lisa DeCamp.
Rather than providing direct medical services, Centro SOL exists to support people like the Mexican-born patient Polk remembers from years ago. Polk was ultimately able to help guide that child toward a surgery that improved her epilepsy, but the whole process was "way too much trial and error," she says, and required a great deal of education for the patient's mother.
"Centro SOL was informed by clinical stories like that," Polk says. "What this child needed was not limited to her medical treatment. She wasn't a citizen, and she needed support for her health and well-being. Her mother did too. Those are the people we envision helping."
Over the fall and winter of 2017, the Sacred Heart of Jesus Church in Highlandtown was rattled by a succession of suicides among its congregants, including a 16-year-old Mexican American boy and a young man from El Salvador.
News reports at the time linked the suicides to a spate of raids across the country by U.S. Immigration and Customs Enforcement, which arrested hundreds of immigrants, including several in Baltimore. Under President Donald Trump, fears of deportation were pervasive—along with anxiety over blatant anti-immigrant rhetoric in the air. Guerrero Vázquez, who was called in by Sacred Heart's pastor to help the community, says the challenges inherent with immigration itself—the distress of resettling, not being able to make enough money—were also weighing heavily on many. She remembers her devastation at hearing that the teenage boy believed he'd be helping his parents if he was no longer around.
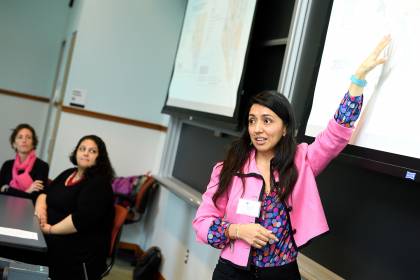
Image caption: Mónica Guerrero Vázquez, executive director of Centro Sol, discusses the organization's work.
Image credit: Will Kirk / Johns Hopkins University
At Sacred Heart, Guerrero Vázquez hosted community meetings to address the trauma, handing out Spanish-language materials and referring to mental health doctors. She paid hospital visits to other congregants who had attempted suicide.
"Mental health is what she's most passionate about," Polk says of Guerrero Vázquez, who was appointed in 2019 to the Maryland Governor's Commission on Suicide Prevention and helped develop Fortalece tu bienestar (Spanish for Strengthen your well-being), an online suicide prevention resource.
A cornerstone of Centro SOL is its Testimonios program, a free weekly mental health support group moderated by bilingual Johns Hopkins psychotherapists or psychiatrists. Pre-pandemic, the groups—separated by gender—met in church rec rooms, with takeout food and child care provided, to talk openly about their stresses, traumas, depression, and loneliness. According to a former Centro SOL researcher Alizay Jalisi, who attended almost 30 sessions, men often worried about supporting their families through informal, low-paying jobs, while many women felt shut out from work opportunities entirely. Some participants spoke of problems with their spouses or domestic abuse, and of struggles with crime in Baltimore.
With that program's success, a teen version was also launched, with social workers gathering groups of Spanish-speaking students every week at 11 Baltimore public middle schools and high schools. Though Teen Testimonios ended during the COVID-19 pandemic, a summer iteration has lived on, helping introduce kids to the city through excursions and activities, along with English lessons. Another program, Summer Scholars, steers academically promising bilingual high schoolers toward careers in medicine, health care, or research.
During the pandemic, Centro SOL moved most of its offerings online. For some programs, including Testimonios, Guerrero Vázquez says the adaptation will likely stick, despite some missing the dinners and personal touch. "I think a lot of what we offer will remain virtual or hybrid because it's just more practical for people to not have to commute," she says. "Right now, I can work with people all over Baltimore without anyone needing to find transportation."
In recent Testimonios sessions, COVID-19 continues to loom large. "Many people have lost family members and they're dealing with loss and grief," says Guerrero Vázquez. Alcohol problems have increased and "financial stability has worsened in families that never had financial stability to start," she says.
In Baltimore and across the U.S., the toll of COVID-19 has been particularly cruel for Latinos. One Brookings Institution study in September 2020 found that Latinos had nearly three times the COVID-19 case counts as whites, and hospitalization rates 4.6 times higher. Half of Latino adults said they had a family member or close friend who'd been hospitalized or died from the virus.
During the pandemic's first wave, physicians at Johns Hopkins were seeing these realities in hospital beds, Page says. Many patients were essential workers—in construction, child care, or the food industry—who had no choice but to continue their jobs during lockdowns. Cramped living conditions also played a part, with household members more likely to pass the virus among themselves.
Centro SOL organized three food distribution sites in Baltimore and a community-based testing clinic at Sacred Heart, which later transformed into a vaccine clinic. Initially, vaccination rates among Latinos were concerningly low, but over time the dynamic shifted—in part owing to advocates like those at Centro SOL, who have worked to dispel myths and assuage fears. "The vaccine rate was very slow to take off, but then it really, really picked up," Polk says. As of December 2021, more than 67% of Baltimore Latinos were vaccinated.
Polk believes a silver lining to the pandemic is that there's no more denying the health needs of Baltimore's Latino community. When hospital beds are filled and health departments are tracking statistics, "no one can say, why do you need a center for Latinos?" she points out. "There's much greater awareness now of their presence in the community and of their health care needs. If you're in treatment for COVID, we learn a lot of other things about you, and we learn more about the complexities of caring for this population."
To this end, Centro SOL pushes for wider representation of Latinos in clinical research studies. In 2020, the center consulted on 21 research projects, helping with recruitment. As Polk says, the focus needs to shift: "How do we not only respond to needs in a crisis but engage in health promotion activities without an emergency?"
With the displacement related to the pandemic, the need is great to meet residents where they live, work, and congregate. During this time Centro SOL has increased its efforts with community health workers—citizens trained to act as a trusted bridge between residents and the health care system—who have ventured into salons, restaurants, and shops to share information about testing and vaccines. At Sacred Heart, CHWs registered neighbors for tests and relayed results over the phone for those without internet. They operated a COVID-19 hotline to answer questions and help with vaccine sign-ups.
"The day-to-day work of COVID response in the Latino community has really been through these CHWs," Polk says. "Usually they share some aspects of the lived experience with the community we're trying to serve."
Guerrero Vázquez says she hopes to develop a model—based on approaches that have worked for disease prevention—that creates a pipeline of CHWs focused on the mental health needs of Baltimore Latinos. "My dream is to have a youth program to train younger CHWs—who can come in, learn with us, then go out and work in the community."
Also see
She's already seen sparks of this potential through Centro SOL's Summer Scholars program. "This one guy in particular actually taught me so much about the challenges you face here as an immigrant youth. He was being told by his teachers, just forget about college," she says—but then graduated from college with an engineering degree and is now pursuing his master's at Morgan State University. She ticks off other successes: One girl pursuing nursing, another neuroscience. "We have so many stories like that."
Someone asked Guerrero Vázquez recently if there could be another Centro SOL in, say, Florida. She's quick to point out the importance of the Hopkins connection to Centro SOL—placing its work at the "crossroads of research and academia and community"—but she does believe the model could be replicable in some way. That's one of the reasons she's now pursuing her doctorate in public health at Johns Hopkins. "I want to build enough capacity to make Centro SOL adaptable to other places," she says. "The work we do—it's very innovative. It's treating people with respect and finding the best ways to serve them."
Posted in Politics+Society
Tagged baltimore, health, health equity, latino health








