On the day Spencer Grace Tully turned 3, doctors told her parents that her brain cancer had stopped responding to treatment. The once happy and seemingly healthy little girl had started experiencing viruslike symptoms at 17 months old, but her condition turned out to be something much worse: medulloblastoma. Surgery and chemotherapy initially rid Spencer of the tumors, but six months after going into remission, the cancer returned, spreading throughout her brain and spine. Radiation therapy would have been debilitating for a child her age and would not have stopped the growth of the cancer for long. They were out of options. "Everything shattered on her third birthday," says Jodi Bosket- Tully, Spencer's mom. "Suddenly, she only had weeks to live."
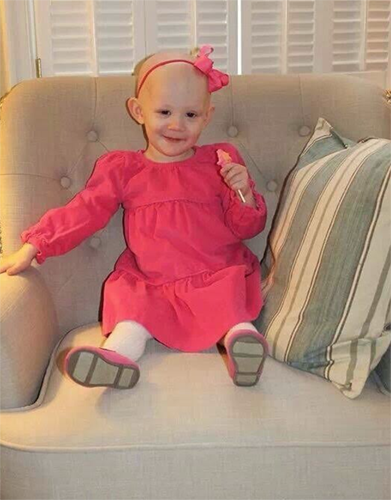
Image caption: Spencer Grace on her last day of chemotherapy before her relapse. "It was a very special day!" says her mother.
Image credit: Courtesy of Jodi Bosket-Tully
Bosket-Tully and husband Chris Tully brought Spencer home for hospice care. As the couple lost hope for a future with their daughter, they vowed to help other families facing a similar loss. "We don't accept what happened to Spencer, or that it could happen to more children," Bosket-Tully says. "If we could help in any way, we wanted to do it."
The couple considered donating Spencer's organs, but they were ineligible because of the aggressive chemotherapy she had received. Spencer's doctors at Johns Hopkins Hospital suggested an alternative: rapid autopsy. Like a standard autopsy, a rapid autopsy involves a pathologist conducting a postmortem examination of the body. But in the case of a rapid autopsy, doctors are also collecting tissue samples to conduct research on how the disease developed and how it might be cured in the future. (Depending on what's agreed upon, it could be an incision to take a sample of a known tumor, or it could be a full-body examination that yields several samples.) At least 10 hospitals in the U.S. currently offer the procedure, and its popularity is expanding, allowing new research on cancer, Alzheimer's disease, HIV, multiple sclerosis, and ALS.
Although the process was entirely unfamiliar to Spencer's parents, when her doctors asked whether they could collect tumor samples after she passed, "it was a very short conversation," Bosket-Tully says. They said yes, and then never asked how the tissue was used. "It was kind of a conscious decision," Bosket-Tully says. "We knew they used it for the research, but what they used it on? We didn't get into the specifics. We just wanted them to use it in whatever way they felt necessary."
Rapid autopsies need to be done soon after death because human tissue begins to degrade immediately. However, when collected quickly—ideally within six hours of death—cells still sufficiently resemble living tissue, says Jody Hooper, an associate professor of pathology and director of the Legacy Gift Rapid Autopsy Program at Johns Hopkins. Scientists can use samples to grow cell lines, sequence DNA or RNA, and test potential new therapies. They're particularly valuable for scientists studying cancer, who can't always collect the tissue samples they need from living patients. Tumors often grow in parts of the body that are difficult to sample, like the brain, or in multiple parts of the body. Sometimes they can't be sampled in large enough quantities for research. And doctors may consider it unethical to subject their patients to procedures such as tumor biopsies if they offer no direct benefit.
Also see
Eric Raabe, an assistant professor of pediatric oncology and pathology in the School of Medicine, says researchers have spent the last 30 years looking for an effective treatment for diffuse intrinsic pontine glioma, or DIPG, an aggressive form of pediatric brain cancer. Most cases of DIPG are diagnosed by MRI instead of tissue biopsy, so there simply wasn't enough tumor tissue for scientists to study. But as rapid autopsy programs expand, says Raabe, more and more families have begun to donate tissue for research.
With a DIPG tumor sample from a rapid autopsy, Raabe's team developed a cell line used by researchers in a dozen labs across three different continents to identify drugs that might work against the disease. Children are now receiving two of these drugs in phase I clinical trials. "It allows patients and families who are not able to beat cancer themselves to make a 'pay it forward' gift to future generations of patients, people who will be affected by that very same cancer," Raabe says.
Bosket-Tully agrees. "It was the best thing we could have done in order to help somebody else. It was the only thing."
Posted in Health, Science+Technology
Tagged pathology, brain cancer








