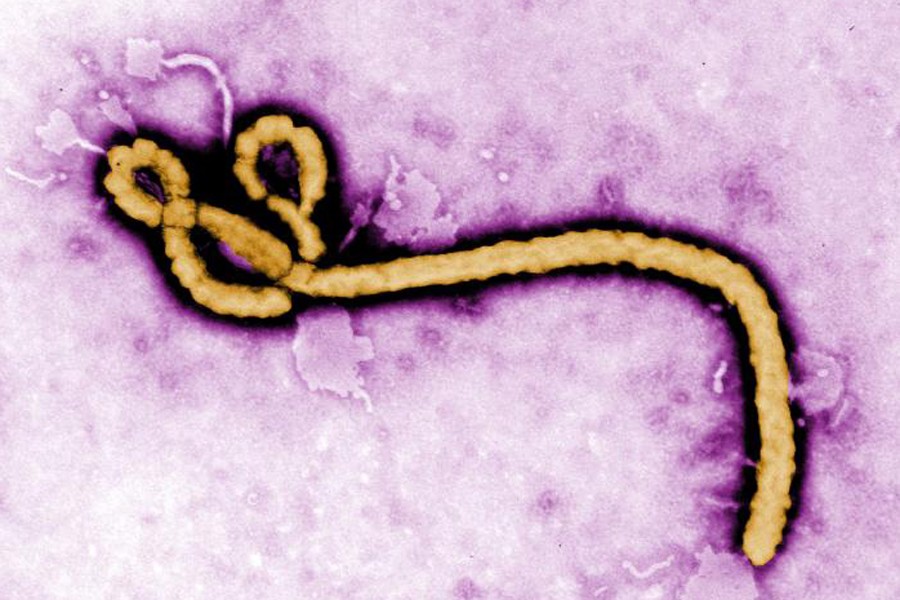
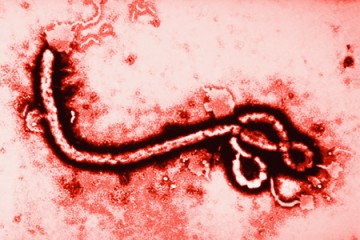
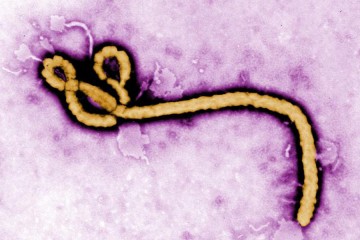
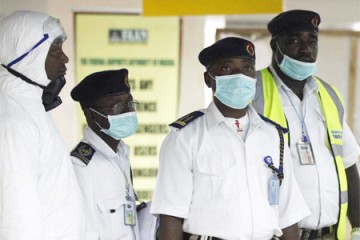
The experimental treatment for the Ebola virus—the so-called "secret serum" being used to treat two American aid workers and a Spanish missionary priest who contracted the disease—has its roots at Johns Hopkins, NBC News reported today.

Image caption: Richard Cone
Mapp Biopharmaceutical, which developed the "plantibodies" used in the treatment, is run by two Johns Hopkins graduates who got their start in the lab of Johns Hopkins biophysics Professor Richard Cone.
From NBC News:
When news broke last week of a Southern California firm's experimental treatment for Ebola, pioneering biophysicist Richard Cone quietly celebrated from his office at Johns Hopkins University. He emailed congratulations to the two former protégés who'd developed the medicine, then allowed himself to dream again.
Cone, 78, runs an esteemed laboratory where for three decades he's been trying to develop a cheap, easy-to-apply antibody treatment for women to prevent unwanted pregnancies and sexually transmitted diseases. It's been arduous, idealistic work that has never attracted investment from venture capitalists or pharmaceutical companies. But he kept at it and learned to accept that he probably wouldn't live to see his life goal realized.
All the while, he watched those former students, Kevin Whaley and Larry Zeitlin, who left his lab in 1999 and went on to form Mapp Biopharmaceutical, where they pursued plants as a way to cheaply and quickly reproduce those antibodies. He rooted them on as they expanded their research to include pathogens that could be used in bioterrorism, such as Ebola, drawing the kind of government attention, and money, that he could only imagine.
Interest in the company suddenly exploded last week, after Mapp allowed two American aid workers infected with Ebola to be treated with its cocktail of antibodies, grown in genetically engineered tobacco plants, that had yet to be tried on humans. The aid workers are reportedly improving, but there's no way to tell yet whether the drug, ZMapp, deserves credit.
ZMapp is made up of specially engineering antibodies—called monoclonal antibodies—that mimic the body's immune response. The drug has never been tested on people, but one of its components—the MB-003 cocktail—resulted in a 43 percent survival rate among infected monkeys, according to an August 2013 article on the journal Science Translational Medicine. That article was co-authored by Zeitlin and Whaley, along with two Johns Hopkins master's in biotechnology graduates—Cara Working, who now works for Kentucky BioProcessing; and Megan Heinrich, who works at the U.S. Army Medical Research Institute of Infectious Diseases.
Also see: Centers for Disease Control Q&A on ZMapp treatment for Ebola virus
"Richard has been both a mentor and a wonderful colleague," Zeitlin wrote in an email to NBC News. "His passion and deep, deep intellect are an inspiration to all who know and love him."
If ZMapp works, Cone told NBC News, it could lead to more support for "plantibodies" research, adding that he hasn't talked to his former students since ZMapp became international news last week.
"I just sent them the emails," he said. "I didn't want to waste their time. I just said, 'good luck.' And hopefully those two patients will recover."
Read more from NBC NewsPosted in Health, Science+Technology
Tagged public health, biotechnology, biophysics, ebola, richard cone